The power of Continuous Glucose Monitors

Introduction
World Diabetes Day is this Thursday, 14th November. This second note focusing on diabetes is more personal. My first experience of diabetes, as some of you may know, was when my older brother, Adrian, was diagnosed with Type 1 when he was 15. We were summoned to hospital as a family to be trained in spotting the difference between hypoglycaemic (low blood glucose) and hyperglycaemic (high blood glucose) events. The family diet changed overnight. My parents had been brought up on the Sunday roast and high tea of mining families. White bread sandwiches, scones and jam and cakes at 4pm were no longer part of our lives. The advice that Adrian was given when diagnosed was far better than the advice that he was subsequently given over time. Initially, there was very much a view that meat and two veg was good and starchy stuff was bad. Sadly, the ‘fat is bad/base your meals on starchy foods’ advice became more strident over the years and Adrian followed that for far longer than he should have done. Adrian would come to stay, and he would be the one having oat biscuits with cheese when Andy and I just had cheese.
All this changed when Adrian was one of the early recipients of a Continuous Glucose Monitor. Within days he was phoning me astonished that he could see for himself what I had been saying for some time – eggs would be better than porridge for breakfast, cheese is better than bread for lunch and you don’t need any starchy carbs at dinner – fill your plate with meat/fish/eggs and/or cheese and vegetables (ideally non-starchy). His life and diet changed in a couple of weeks. He was able to reduce his insulin. He found his blood glucose not only to be lower but more stable. As he reduced insulin, he became less worried about the overnight hypo (which is probably the greatest fear of type 1s). He’s not obsessive about very low carb – he’ll have a set menu in a special restaurant and not worry about it – but he’s routinely substantially lower in carbohydrate than he has been for life.
During the summer of 2018, Andy and I each had the opportunity to try a Continuous Glucose Monitor (CGM) for two weeks. We are not diabetic, but we did it for interest. We made a number of observations. In no particular order they were:
1) ‘Slow release’ carbohydrates
My CGM observations led me to tweet on World Diabetes Day 2018 (Ref 1):
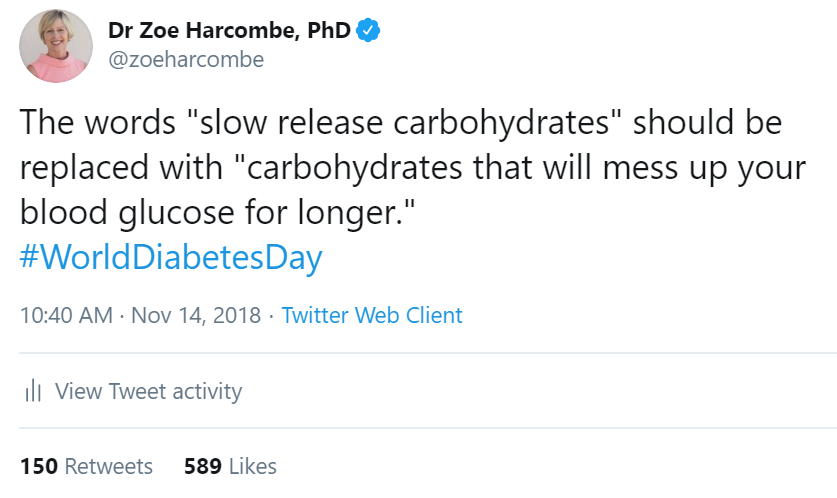
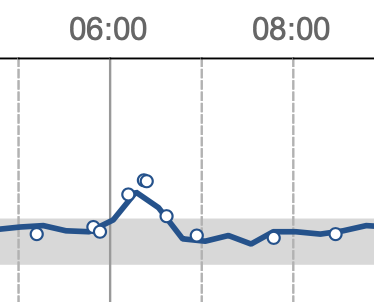
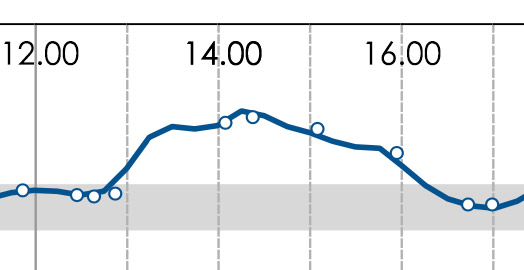
See the graph below when I had a bowl of porridge for lunch to test the impact of slow release carbohydrates. It looks like Table Mountain! Not only did my blood glucose (BG) rise quickly to a high of 13.4, it stayed high between 13.00 and 16.30. (The gray scale in all the charts is the normal BG range – I’ve truncated the daily graphs to focus on the precise example being used).
2) Fruit spikes
In contrast, fruit spikes blood glucose up and down quite quickly (the down quickly is in a non-diabetic – fruit would be more problematic in a diabetic person). I typically enjoy full fat dairy (yoghurt and milk) for breakfast with some berries. I like an orange too. The days I had the orange, my BG would spike up as high as 10 or 11 and then come down. On the days when I had the yoghurt, milk and berries without the orange, I stayed nicely within the normal BG range.